By Dr Nosa Efeovbokhan
•
March 6, 2026
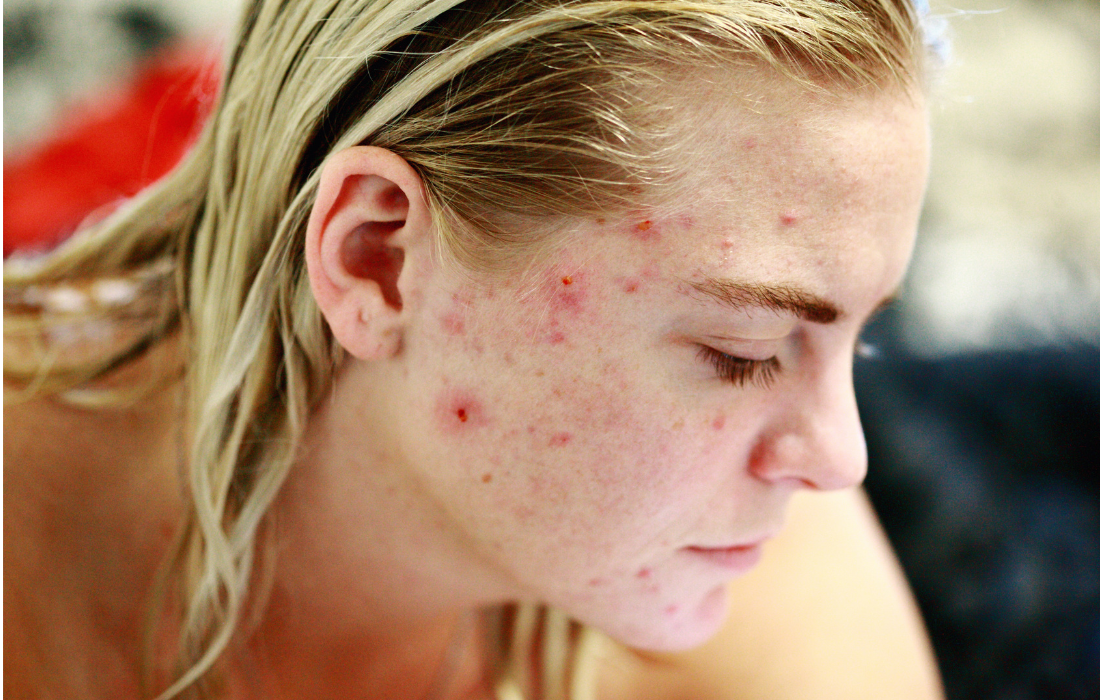
Not everyone faces the same chance of developing skin cancer. Some people carry an elevated skin cancer risk because of their genes. Others build it up slowly through years of outdoor exposure and sun habits. Most people do not know where they sit on that risk scale. That gap in awareness is where harm happens. Knowing your personal skin cancer risk is one of the most useful things you can do for your long-term health. It shapes how often you need regular skin checks , which sun safety tips apply most to you, and what skin condition care your GP recommends. At Molonglo Valley Medical Centre, we evaluate this risk as a routine part of skin health molonglo valley patients access through our practice. This guide explains every major risk factor in plain terms. Why Skin Cancer Risk Varies From Person to Person Skin cancer is the most diagnosed cancer in Australia each year. The numbers are significant. But within that broad statistic, individual risk varies widely. Two people living in the same suburb, doing the same job, can carry very different levels of skin cancer risk . That variation comes from a mix of genetics, skin biology, life history, and daily choices. None works alone. They combine and grow over time. Knowing which factors apply to you helps your GP at Molonglo Valley Medical Centre build the right care plan for your skin. Genetic and Biological Risk Factors Some skin cancer risk factors are set before you are born. They come from your genes and your skin biology. You cannot change them. But you can plan around them. Skin Tone and Sun Response Skin that reddens quickly in the sun without building much of a tan holds less natural UV protection than darker skin tones. This does not mean people with darker skin have no risk. UV damage affects all skin types. But the risk level differs, and the monitoring plan your GP sets will reflect that. People whose skin burns in less than 15 minutes of midday sun sit at the higher end of the biological risk range. Eye and Hair Colour Light-coloured eyes — grey, pale green, or pale blue — are linked to lower melanin levels across the whole body, including the skin. Hair that is naturally fair, red, or copper-toned tends to come with the same lower-melanin profile. Both are biological markers of higher your risk . Mole Count and Type Having many moles on your body elevates your skin cancer risk . This is especially true when those moles are large, uneven in shape, or mixed in colour. Moles that look different from one another on the same body are also worth watching closely. Your GP documents and images these at your regular skin checks visits. The number alone matters too. People with over fifty moles sit in a higher-risk group regardless of whether any individual mole looks unusual. Family History of Melanoma If a parent, brother, sister, or child has been treated for melanoma, your own risk is meaningfully higher. This is not just about shared genetics. Families often share sun habits, outdoor lifestyles, and the same UV environment over many years. Tell your GP if any close family member has had a melanoma diagnosis. It directly changes how often you should book regular skin checks . Sun Exposure History: How the Past Shapes Today's Risk Every hour of unprotected sun your skin has absorbed over your lifetime has left a mark. That mark is invisible until it is not. UV damage does not show up right away. It builds slowly over years before it becomes visible. This is why skin cancer risk rises with age. It is also why what you do today still matters, even if the damage so far has come before you thought about sun safety. Severe Burns During Childhood and Youth Intense sun burns during early life leave a mark on skin cells that persists for decades. A person who had several severe burns before the age of 18 carries a higher skin cancer risk into adulthood, regardless of how careful they have been since. Children in Molonglo Valley grow up in a high-UV environment. Protecting them now is one of the most effective long-term cancer prevention steps a parent can take. Outdoor Work and Outdoor Lifestyles People who spend most of their working day outside accumulate far more UV than office workers over the same period. Tradies, landscapers, teachers with outdoor duties, coaches, and farmers are among the groups with the highest skin cancer risk from occupational exposure. An active outdoor leisure life adds to this. Weekend sport, gardening, and trail walking all count toward the total UV your skin has carried. UV Tanning Equipment Using a UV tanning bed at any point in your life adds to your skin cancer risk . This is true even for brief or infrequent use. Tanning bed UV is often stronger than natural sunlight. It drives the same DNA damage that outdoor exposure causes. There is no safe dose of artificial UV tanning. If you have used this equipment in the past, mention it to your GP when discussing your risk profile. Medical History and Immune Function Your medical background also shapes your skin cancer risk . Some health conditions and treatments change how your immune system handles UV-damaged cells. Immune System Strength A strong immune system catches and clears damaged skin cells before they can grow into cancer. When the immune system is low, that process becomes less reliable. People taking long-term medicines that lower immune response — such as those used after organ transplants or for certain autoimmune conditions — face a higher skin cancer risk . If this applies to you, your GP will recommend a closer schedule of regular skin checks than the standard recommendation. Previous Skin Cancer Diagnosis Skin that has produced cancer once has shown a pattern worth watching. People with a past skin cancer diagnosis are among the highest-priority groups for regular skin checks . Most move to a six-monthly or more frequent schedule. All three types — melanoma, basal cell, and squamous cell — increase the chance of a future growth. The type shapes the monitoring plan. The Molonglo Valley Factor: Local UV and Lifestyle Skin health molonglo valley residents need to prioritise carrying a local dimension that many people underestimate. Canberra sits at a higher altitude than most major Australian cities. Less atmosphere above means less natural UV filtering. The UV load reaching the ground is stronger than many residents expect, especially during spring and summer. Molonglo Valley is also an outdoor suburb. Parks, walking paths, sports ovals, and school grounds are used daily by residents of all ages. That regular outdoor time adds up to a real UV exposure figure each week. For families in Coombs, Wright, Whitlam, and Denman Prospect, building good sun habits is not just sound advice. It is a practical response to the UV environment in which they actually live. Sun Safety Tips That Match Your Risk Level Good sun safety tips are not one-size-fits-all. The higher your skin cancer risk , the more careful your daily cover needs to be. The ARPANSA UV monitoring tool shows the daily UV reading for your area. When the reading reaches three or higher — which happens regularly in Canberra across most of the year — protective steps are needed. Daily Protection Habits That Make a Real Difference • Cover exposed skin with clothing that has a close weave. Long sleeves and a collar do more for your skin than any cream • Apply SPF 30 or higher sunscreen each morning before leaving the house. Do not wait for warm weather to start • Wear a hat with a brim that drops on all sides. A front-peak cap leaves your neck, ears, and cheeks without cover • Stay in the shade between mid-morning and early afternoon. These are the hours when UV sits at its peak each day • Choose wrap-style sunglasses with UV-rated lenses to guard the eyes and the thin skin that surrounds them Getting Your Sunscreen Use Right Most people use far less sunscreen than the tested dose. A thin layer does not deliver the protection shown on the bottle. Apply it well and give it around 20 minutes before going outside. Put it on again after swimming, after you have sweated heavily, or once two hours have passed since your last application. Sunscreen is one tool in your sun safety tips plan. It works best alongside clothing and shade, not as a replacement for them. Sun Safety Tips for Children in High-Risk Families Children who carry genetic risk factors — fair skin, red hair, a family history of melanoma — need more careful sun protection than their peers. High-factor sunscreen, a proper hat, and shade breaks during peak UV hours are the baseline. Start these habits early. They become automatic when built into childhood routines. Talk to your GP about whether your child should start regular skin checks earlier than the general population recommendation. Regular Skin Checks: Your Early Warning System Knowing your skin cancer risk level is the first step. Acting on it is the second. Regular skin checks give your GP a professional, magnified view of your skin at a set interval. They are the most reliable way to catch changes before they become serious. At Molonglo Valley Medical Centre, each skin check includes digital imaging that creates a baseline record. Your doctor compares that record at every visit. Slow shifts in a mole or spot that would be easy to miss are visible in that comparison. How Risk Level Shapes Your Check Schedule • Low risk, no relevant history: a check every two years keeps you covered • Standard adult risk with outdoor exposure: once a year is the baseline we recommend • Fair skin, high mole count, or a removed lesion: six-monthly visits suit your profile • Past melanoma or close family history: three to six months, guided by your GP after your first assessment What to Watch for Between Visits A monthly home check trains you to know what is normal on your own skin. Look for moles where the two sides do not sit evenly. Watch for any spot with an edge that has become less defined. Flag a colour that blends more than one shade in one small area. Note anything that has grown noticeably. And treat any lesion that itches, bleeds, or will not settle as a prompt to book in before your next scheduled visit. Skin Condition Care and Skin Cancer Risk: Managing Both Together Some skin conditions change how easy it is to spot a new or changing lesion. Patches, redness, and scale can hide what sits underneath. If you manage eczema, psoriasis, or another ongoing skin condition, regular skin checks become even more useful. Your GP reviews your skin condition care and screens for cancer in the same appointment. At Molonglo Valley Medical Centre, skin condition care and skin cancer risk management sit side by side. You do not need to choose between them or book two separate visits. Complete Your Skin Health Reading This blog covers skin cancer risk in depth. For the full picture of skin health in Molonglo Valley, read Other pillar guide: → Your Complete Guide to Skin Health in Molonglo Valley – Prevention, Checks & Care The Full Skin Health Blog Series → Skin Health and Cancer Prevention in Molonglo Valley: What Every Resident Should Know → Why Regular Skin Checks Are Critical: Early Detection, What Doctors Look For & How Often → Common Skin Conditions Explained: Acne, Eczema, Psoriasis & When to See Your GP Frequently Asked Questions Q1. I have fair skin and several moles. Does that automatically make my skin cancer risk high? Fair skin and a high mole count both raise your risk above the average. But risk is not just one number — it is a picture built from several factors together. Your GP at Molonglo Valley Medical Centre looks at your full profile: skin tone, mole count, family history, sun exposure record, and any past skin concerns. From that combined picture, they set the right monitoring schedule for you. Book a skin check and get a clear answer rather than guessing. Q2. I used a tanning bed occasionally in my 20s. Should I mention this to my GP? Yes, always mention it. Any use of UV tanning equipment raises skin cancer risk , even if it was occasional and many years ago. UV delivered through a tanning bed often runs at a higher concentration than midday outdoor sun. The skin damage it causes is the same kind that builds toward cancer over time. Your GP will factor this into your risk assessment and may recommend starting regular skin checks sooner or more frequently than someone without that history. Q3. My father had melanoma. How does that affect my own skin cancer risk and what should I do? A melanoma diagnosis in a close family member is one of the most significant individual risk factors your GP considers. Your own skin cancer risk is meaningfully higher than someone without that family history. The right response is to book a skin check at Molonglo Valley Medical Centre if you have not had one recently. Your GP will assess your full risk profile and put a monitoring schedule in place. In most cases with a parent’s melanoma history, annual checks are the minimum — and more frequent visits may be recommended. Q4. I work outdoors every day. What sun safety tips should I prioritise above everything else? Physical cover is the highest priority for outdoor workers. A long-sleeve, close-weave shirt and a hat with a full brim reduce your UV exposure more than sunscreen alone. Apply SPF 30 or higher sunscreen to any skin that clothing does not cover, and reapply it after heavy sweating. Step into shade at lunch when UV sits at its daily peak. Book an annual skin check so your GP can track what the exposure is doing to your skin over time. Outdoor work is one of the strongest lifestyle contributors to skin cancer risk , so the monitoring matters as much as the daily habits. Q5. Can I get both a skin condition review and a skin cancer check in the same visit? Yes. This is something our GPs do regularly at Molonglo Valley Medical Centre. Patients managing eczema, psoriasis, or acne often have skin cancer screening folded into the same appointment. Let reception know when you book that you want to cover both your ongoing skin condition care and a skin cancer risk check. We will allocate enough time for both. You leave with a treatment update and a full cancer screening done in a single visit. Take Action on Your Health Today Your health matters at every stage of life. From routine check-ups and preventive care to managing ongoing health concerns, early medical support can make a real difference. At Molonglo Valley Medical Centre, our experienced GPs provide professional, compassionate care for individuals and families in a comfortable environment. 📅 Book your appointment today 02 5110 3155 https://www.molonglovalleymedicalcentre.com.au/contact